Healthcare transition represents one of the most significant challenges that families managing rare diseases face. As children with complex medical conditions mature into adults, the shift from paediatric to adult healthcare systems requires extensive preparation, careful coordination, and early planning to ensure continuity of care.
The transition process involves moving from a family-centred, paediatric model of care to an adult healthcare system that emphasises patient autonomy and self-management. For families dealing with rare diseases, this transition is particularly complex due to the specialised nature of the required care and the limited number of adult specialists familiar with these conditions.
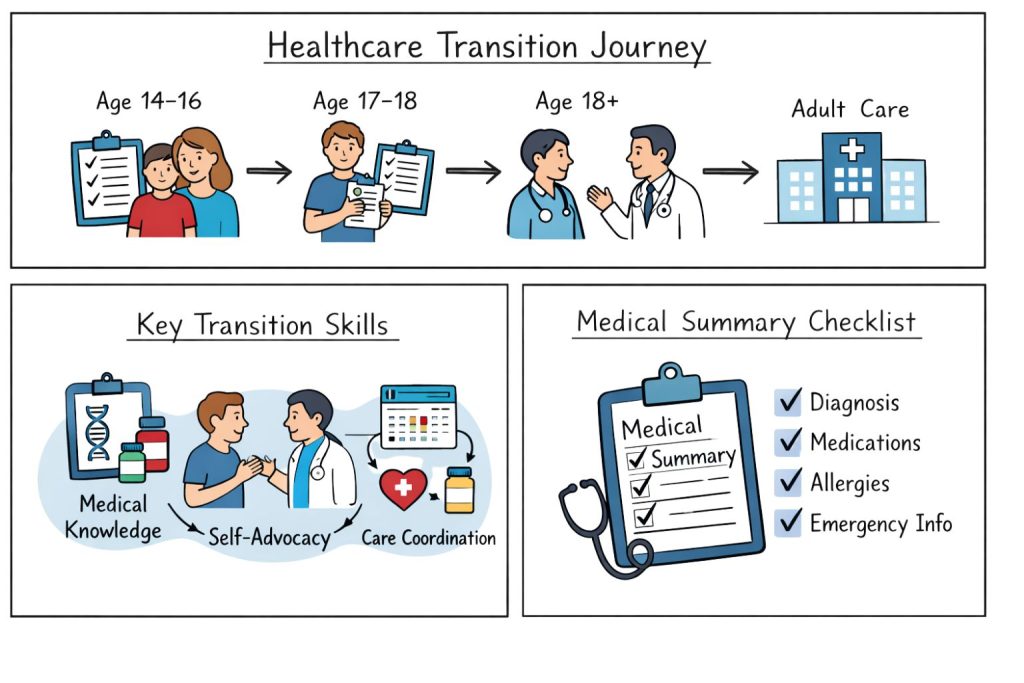
Healthcare transition encompasses the purposeful movement of adolescents and young adults from child-centred to adult-oriented healthcare systems. This process extends beyond simply changing doctors as it requires developing new skills, understanding different care philosophies, and navigating entirely different healthcare structures.
For patients with rare diseases, successful transition becomes particularly critical. Many paediatric specialists have extensive experience managing rare conditions in children, while adult healthcare providers may have limited exposure to these same conditions. This knowledge gap can create significant challenges during the transition period.
Research indicates that 18 to 21 years represents the optimal age range for completing healthcare transition, though preparation should begin much earlier. The American Academy of Paediatrics recommends starting transition planning by age 14, with initial discussions beginning as early as age 12.
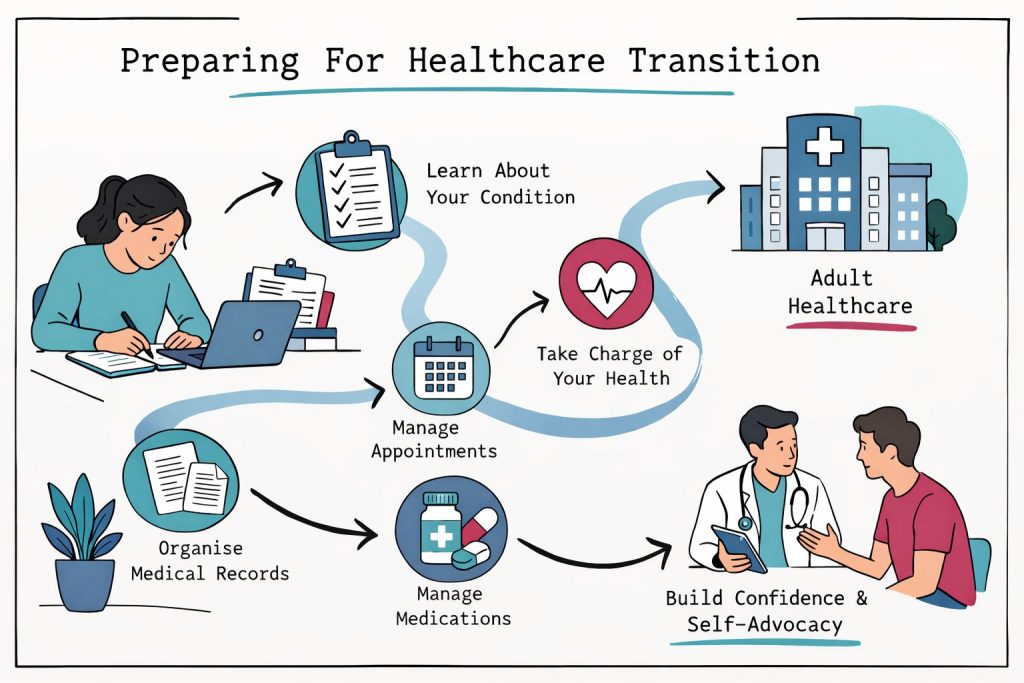
Early preparation is essential when managing rare diseases for several factors unique to these conditions. Complex treatment regimens, multiple specialist appointments, and sophisticated care coordination requirements cannot be transferred overnight.
Families managing rare diseases often develop intricate support networks over years of care. These networks typically include multiple specialists, therapists, social workers, and community resources. Replicating this level of coordination in adult healthcare systems requires planning and gradual skill development.
The paediatric healthcare model emphasises family involvement in all aspects of care planning and decision-making. Parents typically serve as primary advocates, coordinators, and information sources for their children's medical teams. Adult healthcare systems, conversely, expect patients to assume these responsibilities independently.
Young adults with rare diseases must develop comprehensive self-advocacy skills, including the ability to articulate complex medical histories, coordinate between multiple providers, and make informed healthcare decisions. These skills require time and practice to develop effectively.
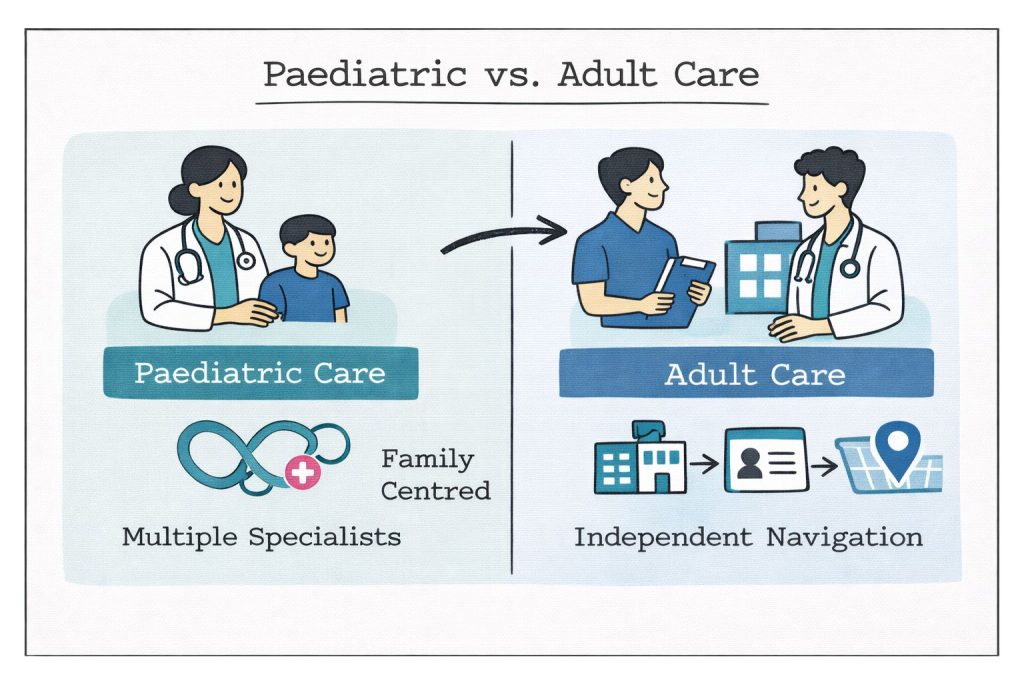
Understanding the fundamental differences between paediatric and adult healthcare approaches helps families prepare for transition more effectively. These differences extend beyond patient age to encompass care philosophy, service delivery, and patient expectations.
Paediatric care operates on a family-centred model, with parents and caregivers playing central roles in medical decision-making. Healthcare teams typically communicate with both patients and families, recognising that children and adolescents are developing decision-making capabilities gradually.
Adult healthcare emphasises individual autonomy and patient responsibility. Adult providers expect patients to communicate independently, make informed decisions, and manage their healthcare proactively. This shift requires significant adjustment for young adults accustomed to shared decision-making.
Paediatric healthcare systems often provide comprehensive care coordination through dedicated case managers, social workers, and nurse coordinators. Many paediatric facilities offer integrated services, including therapy, mental health support, and family resources, all in a single location.
Adult healthcare systems typically require patients to coordinate services independently across multiple providers and locations. While case management exists in adult settings, it operates differently and may not provide the same level of comprehensive support that families experience in paediatric care.
Many rare diseases have dedicated paediatric specialists with extensive experience managing these conditions in children. Adult specialists familiar with rare diseases may be fewer in number and geographically dispersed, potentially requiring travel or making remote consultation arrangements.
Successful transition requires systematic development of healthcare management skills over time. The transition readiness assessment should evaluate multiple domains, including medical knowledge, self-advocacy abilities, and practical healthcare management skills.
Young adults must develop a comprehensive understanding of their rare disease, including genetic basis, symptoms, treatments, and potential complications. This knowledge enables effective communication with new providers and informed participation in treatment decisions.
Medication management is a critical skill that requires gradual development. Patients need to understand dosing schedules, potential side effects, drug interactions, and the importance of adherence. For rare diseases with complex treatment regimens, this knowledge becomes particularly important.
Effective communication with healthcare providers requires specific skills, including accurately describing symptoms, asking relevant questions, and clearly expressing concerns or preferences. Young adults must also learn to advocate for appropriate care and seek second opinions when necessary.
Developing these communication skills requires practice in controlled environments before the full transition occurs. Many paediatric providers encourage a gradual increase in direct patient communication during adolescent years as preparation for adult care.
Adult healthcare systems require patients to navigate complex insurance requirements, scheduling procedures, and to coordinate with multiple providers independently. These skills require systematic development and practice before full transition.
Understanding insurance coverage, prior authorisation requirements, and appeals processes becomes particularly important for rare disease management, where treatments may be expensive or require special approval.
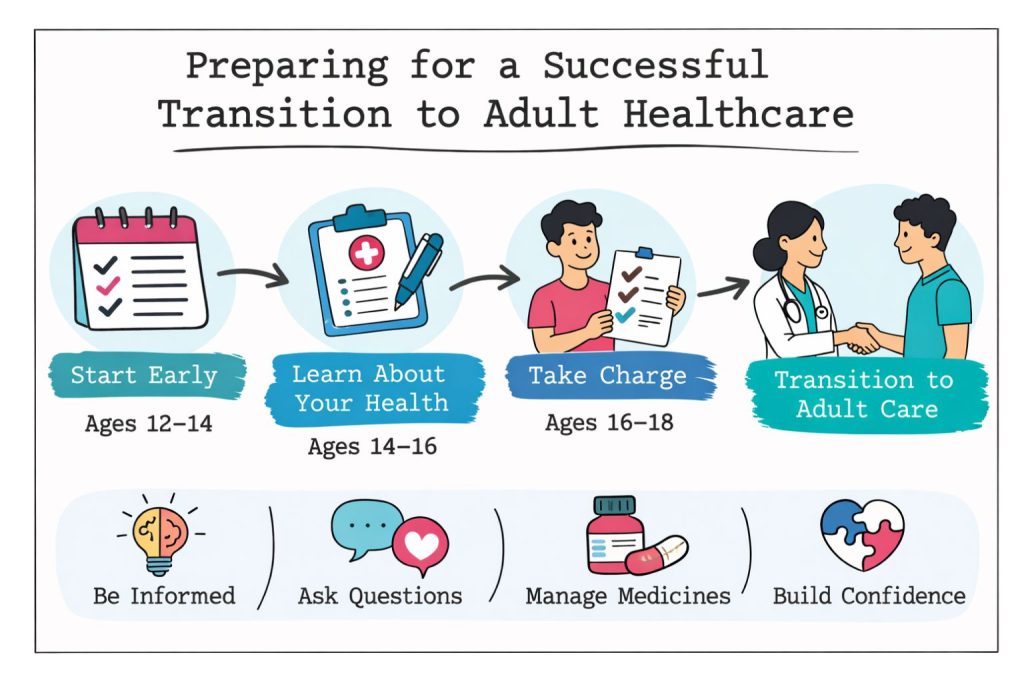
Effective transition planning requires a systematic approach beginning several years before the actual transfer to adult care. This planning process should involve patients, families, current healthcare teams, and prospective adult providers when possible.
The recommended timeline begins with initial discussions at age 12-14 and progresses through structured preparation activities. By age 16, families should identify potential adult providers and begin establishing relationships when possible.
Ages 14-16 represent critical years for skill development, including independent attendance at appointments, direct communication with providers, and gradual assumption of healthcare management responsibilities.
Ages 17-18 require intensive preparation, including compiling comprehensive medical records, identifying adult providers, and completing transition assessments to identify remaining skill gaps.
Comprehensive medical record compilation is particularly important for patients with rare diseases, whose complete medical histories may not be readily available to new providers. This compilation should include diagnostic test results, treatment responses, and detailed care plans.
Creating portable medical summaries highlighting key information enables effective communication with new providers and emergency care teams. These summaries should include diagnosis details, current medications, allergies, and emergency care instructions.
Identifying appropriate adult providers requires research into specialist availability, expertise with specific rare diseases, and institutional resources. This process may require consultation with current paediatric teams and rare disease organisations.
When possible, establishing relationships with adult providers before full transition allows a gradual introduction and knowledge transfer. Some programs offer joint appointments during transition periods to facilitate continuity.
Families managing rare diseases encounter specific challenges during healthcare transition that require proactive planning and problem-solving. Understanding these challenges enables better preparation and more successful outcomes.
The scarcity of adult providers experienced in specific rare diseases poses a significant challenge that requires creative solutions. Families may need to travel longer distances or establish care relationships with providers willing to learn about unfamiliar conditions.
Maintaining relationships with paediatric specialists for consultation purposes may provide valuable support during the early transition period. Some providers offer informal consultation to adult colleagues managing former paediatric patients.
Healthcare transition often coincides with insurance coverage changes as young adults age out of paediatric policies or transition to independent coverage. These changes may affect provider networks, medication coverage, and treatment access.
Understanding insurance options and coverage requirements before transition enables better planning and reduces treatment disruptions. This preparation becomes particularly important for patients with rare diseases who require expensive medications or specialised treatments.
The emotional aspects of healthcare transition often receive insufficient attention despite their significant impact on transition success. Young adults may experience anxiety about assuming healthcare responsibility or grief about leaving familiar providers and systems.
Families benefit from acknowledging these emotional aspects and developing coping strategies. Mental health support during transition periods can facilitate better adjustment and long-term success.
Healthcare transition research continues evolving with increasing recognition of its importance for rare disease populations. Improved transition programs, better adult provider training, and enhanced care coordination tools represent areas of ongoing development.
Successful transition outcomes depend on collaborative efforts between paediatric and adult healthcare systems, patient advocacy organisations, and families managing rare diseases. Early preparation, systematic skill development, and comprehensive planning provide the foundation for successful healthcare transition and optimal long-term outcomes.
The investment in thorough transition preparation pays dividends through improved health outcomes, reduced healthcare disruptions, and enhanced quality of life for young adults managing rare diseases throughout their adult years.