For individuals living with rare diseases, accessing specialised medical care can feel overwhelming and, at times, out of reach. Traditional healthcare systems require extensive travel, multiple appointments with unfamiliar clinicians, and significant financial strain to obtain appropriate care. Telehealth is reshaping this reality by enabling remote access to specialist expertise, bringing high-quality care directly into patients’ homes.
The scale of the challenge is significant. According to a 2019 survey conducted by the National Organization for Rare Disorders (NORD), nearly 40% of people with rare conditions and their caregivers must travel more than 60 miles to consult a clinician with relevant expertise. In many regions, limited exposure to rare diseases means local providers may lack the specialised training required to recognise complex and variable symptom patterns, often contributing to delayed diagnosis and fragmented care pathways.

Telehealth encompasses a broad range of technologies that enable remote delivery of healthcare services. For individuals living with rare diseases, this includes virtual consultations with specialist clinicians, remote monitoring of symptoms and vital signs, digital health platforms for clinical trial participation, and coordinated care across multiple providers.
These services are delivered through secure video consultation systems, mobile health applications, and integrated electronic health records, allowing real-time access to and sharing of medical information. Through these technologies, patients can connect with geneticists, neurologists, oncologists, and other subspecialists without geographic limitations.

Remote monitoring tools further enhance care by allowing ongoing tracking of disease progression and treatment response. Data collected through wearable devices, smartphone applications, and home-based medical equipment can be reviewed by healthcare professionals to support timely, informed adjustments to treatment plans.
Telehealth removes one of the most significant barriers to rare disease care: distance. Patients experiencing mobility challenges, chronic fatigue, or compromised immune systems can access specialist consultations without the physical strain and health risks associated with travel.
The benefits extend beyond patients' families and caregivers. Virtual appointments reduce the need for time away from work, childcare arrangements, and complex travel planning, making routine follow-up care far more manageable.
The limited availability of rare disease expertise becomes far less restrictive when care is no longer tied to location. Telehealth platforms allow patients to connect with leading specialists worldwide, whether they are based in major academic hospitals or international research centres.
Video-enabled consultations also support multidisciplinary care. Patients with complex conditions can engage with multiple specialists, such as geneticists, neurologists, and metabolic experts, from different countries within a single, coordinated appointment.
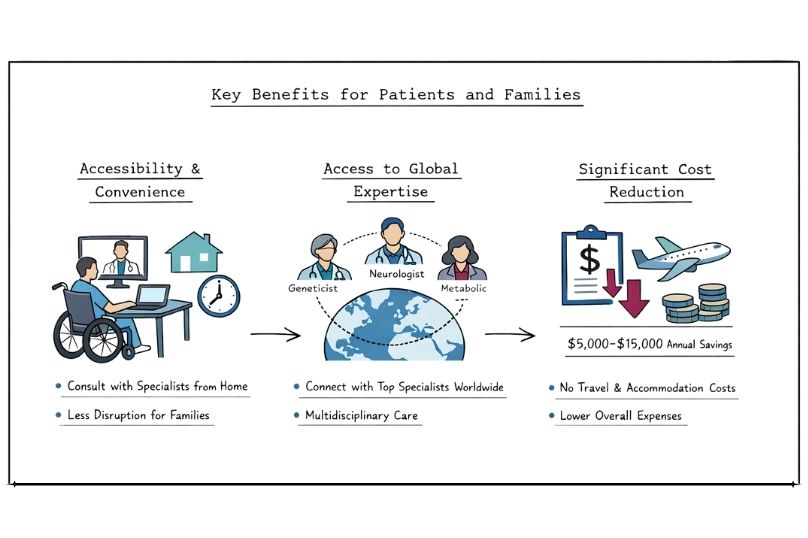
The financial impact of telehealth extends well beyond direct care fees. Traditional rare disease care often requires substantial out-of-pocket expenses for travel, accommodation, meals, and lost income. A single consultation appointment can easily cost families several thousand dollars in associated expenses.
Remote care eliminates these costs while maintaining the same level of specialist expertise. Many families report annual savings of between $5,000 and $15,000 when transitioning from traditional in-person specialist care to hybrid telehealth models.
Telehealth accelerates the diagnostic process through collaborative consultation platforms. Multiple specialists can review patient records, imaging studies, and laboratory results simultaneously, helping shorten the time from initial assessment to an informed diagnosis.
Digital health tools also support the structured collection of patient-reported outcomes and ongoing symptom tracking. This comprehensive information helps clinicians to recognise patterns and clinical links that may not emerge during limited in-person appointments.
Remote enrolment and monitoring options dramatically expand clinical trial participation opportunities for people affected by rare diseases. Patients living in rural areas or regions without major research centres can participate in cutting-edge clinical studies without the need for relocation or frequent travel.
Digital platforms facilitate remote consent processes, electronic data capture, and virtual study visits. These approaches help overcome long-standing recruitment challenges in rare disease research by widening the pool of eligible participants.
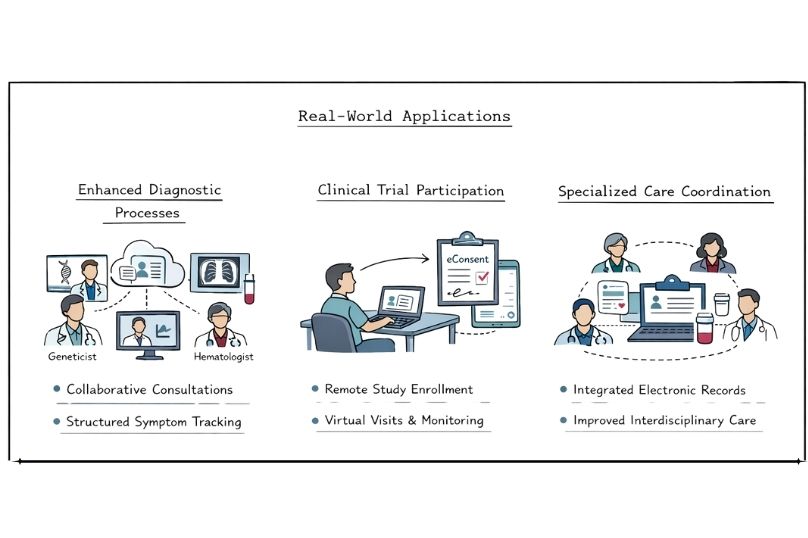
Complex rare diseases often require input from several specialist clinicians. Telehealth platforms facilitate effective communication and shared access to information across care teams, ensuring a consistent and coordinated approach to care.
Integrated electronic records provide clinicians with access to current patient information, enabling informed decisions, reducing the risk of medication interactions, unnecessary testing, and conflicting treatment recommendations.
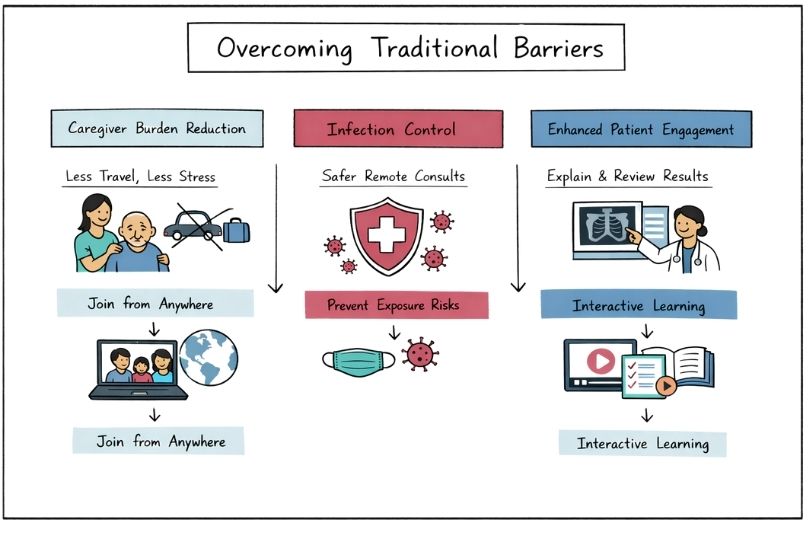
Caregivers often experience significant stress reduction when telehealth options are available. The elimination of travel requirements decreases both physical and emotional strain on families managing complex rare conditions.
Virtual appointments enable family members to participate in consultations without geographical constraints, improving family communication and shared decision-making processes.
Immunocompromised patients with rare diseases face heightened infection risks in clinical settings. Telehealth offers a safer option for accessing specialist care while minimizing exposure to hospital-acquired pathogens.
During infectious disease outbreaks or seasonal flu periods, remote consultations ensure continuity of care without compromising patient safety.
Virtual platforms enable providers to spend more time explaining complex medical information and ensuring patient understanding. Screen sharing capabilities allow real-time review of test results, imaging studies, and treatment options.
Digital health tools facilitate patient education through interactive modules, video resources, and downloadable materials that patients can review at their own pace.
Significant disparities exist in access to technology and digital literacy skills among patient populations. Rural communities, elderly patients, and low-income families may lack reliable internet connections or appropriate devices for telehealth participation.
Healthcare systems must address these equity issues through measures such as device lending programs, technical support services, and alternative ways to deliver care for underserved populations.
State licensing requirements, interstate practice regulations, and insurance reimbursement policies create ongoing barriers to telehealth implementation. Providers must navigate complex regulatory frameworks that vary by location and insurance coverage.
Policy modifications would ensure sustainable funding for telehealth services and remove structural barriers that restrict patient access to remote care options.
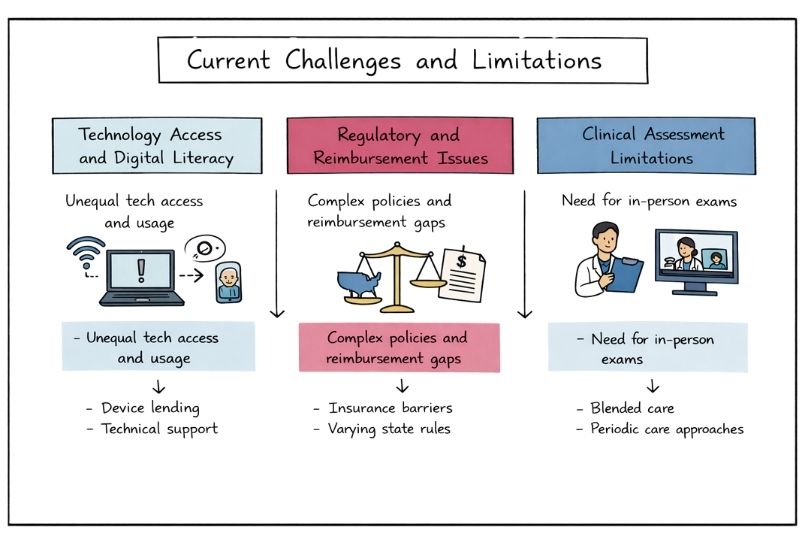
Certain aspects of medical evaluation require physical examination that cannot be fully addressed through virtual consultations. Healthcare professionals must carefully determine which clinical scenarios are appropriate for remote assessment and when in-person evaluation remains necessary.
Blended care approaches, combining telehealth consultations with periodic in-person visits, often provide the optimal balance between convenience and comprehensive clinical assessment.
Artificial intelligence integration promises to enhance telehealth capabilities through automated symptom analysis, predictive analytics for disease progression, and personalised treatment recommendations based on large datasets.
Progress in wearable technologies will enable more sophisticated remote monitoring options, allowing continuous tracking of disease biomarkers and treatment response indicators outside traditional care settings.
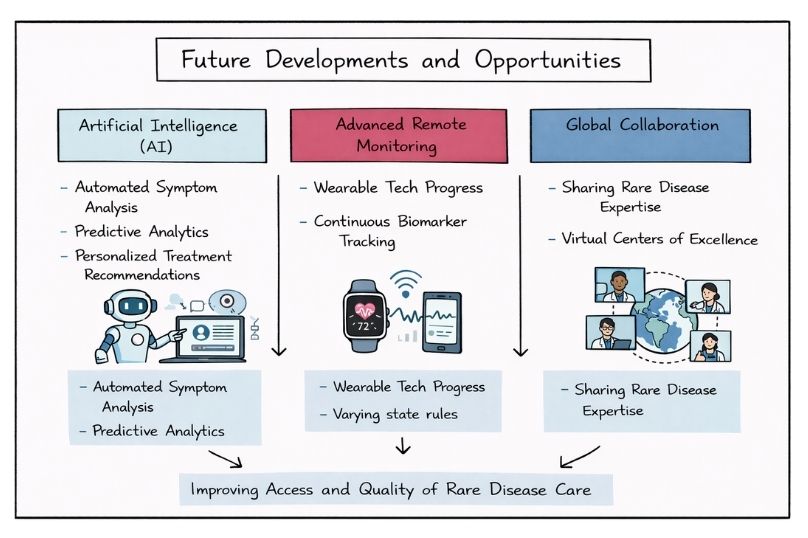
International collaboration platforms will facilitate sharing global rare disease expertise, creating virtual centres of excellence that transcend geographic boundaries.
The transformation of rare disease care through telehealth represents a fundamental shift toward patient-centred and more accessible healthcare delivery. As technology continues to advance and regulatory barriers are addressed, remote care is likely to become a core element of comprehensive rare disease management. This evolution promises to reduce patient isolation and long-standing access challenges that have historically defined the rare disease patient experience, creating new possibilities for improved health outcomes and quality of life.