Support your child’s mental health through chronic illness by recognizing that rare diseases affect far more than physical health alone. Children living with rare diseases often face psychological challenges that extend far beyond their symptoms. The constant uncertainty, complex medical routines, and lifestyle limitations can take a significant emotional toll. Providing thoughtful, informed support strategies is essential to help young patients build resilience and maintain emotional well-being throughout their journey.
Research shows that children with chronic illnesses, including rare disease conditions, experience higher rates of anxiety, depression, and behavioral challenges compared to their healthy peers. For families navigating rare diseases, coping as a family after a rare disease diagnosis often includes understanding and addressing key aspects of children’s mental health, which is essential to providing comprehensive emotional support and care.
Living with a chronic illness (rare disease) can deeply affect a child’s emotional and psychological development. Unlike short-term illnesses that resolve with treatment, rare diseases often bring ongoing uncertainty, complex medical routines, and unpredictable symptom patterns that can significantly impact psychological development and everyday functioning.
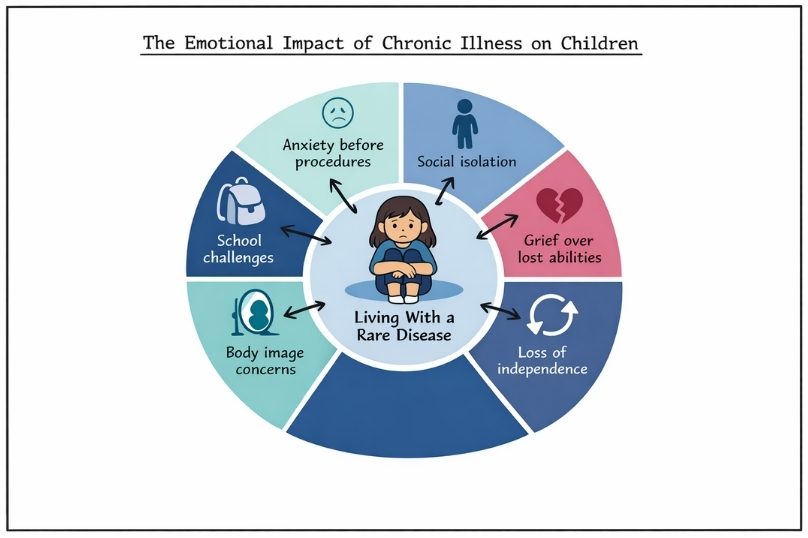
Children with rare diseases commonly experience anticipatory anxiety before medical procedures, feelings of social isolation because of activity limitations, and grief over abilities they have lost or plans that have changed. Importantly, these emotional reactions are not signs of a psychological disorder that needs immediate clinical treatment; they are natural responses to extraordinary circumstances. Recognizing them as part of the adjustment process helps families and care teams provide support without pathologizing normal emotional adaptation.
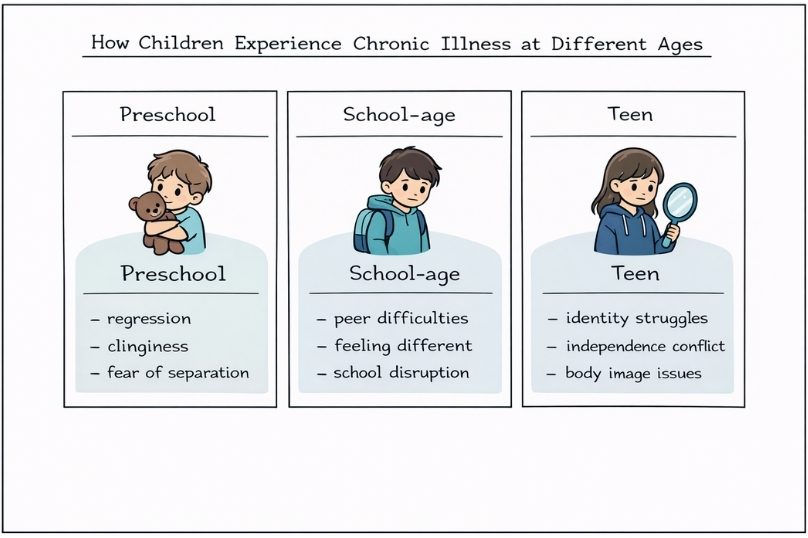
A child’s age and stage of development play a big role in how they understand and cope with their condition.
Preschoolers may show regression in skills they had already mastered, such as toilet training or speech.
School‑age children often struggle to maintain peer relationships and feel “different” from their friends when illness limits their participation in everyday activities. Adolescents frequently face challenges with identity formation, independence, and body image while managing the realities of their medical condition.
The concept of illness intrusiveness describes how chronic conditions interfere with valued activities, relationships, and future goals. For children with rare diseases, this interference can feel especially strong because symptoms are often complex and unpredictable, making it harder to plan and participate fully in normal life experiences.
One of the most effective ways to help your child build emotional resilience is through clear, age-appropriate education about their condition.
Children who understand their rare disease in simple, honest terms usually adjust better emotionally and cooperate more willingly with treatment. This understanding should grow gradually as your child develops, with explanations that match their age and cognitive level.
Effective illness education goes beyond naming the diagnosis. It involves explaining symptoms, the reasons behind treatments, and setting realistic expectations about outcomes. Specialists in child development recommend using simple language, everyday words, pictures, diagrams, and hands‑on demonstrations to make complex medical information easier to grasp. By helping children make sense of what is happening to their bodies, families and care teams provide a foundation for confidence, trust, and emotional strength.
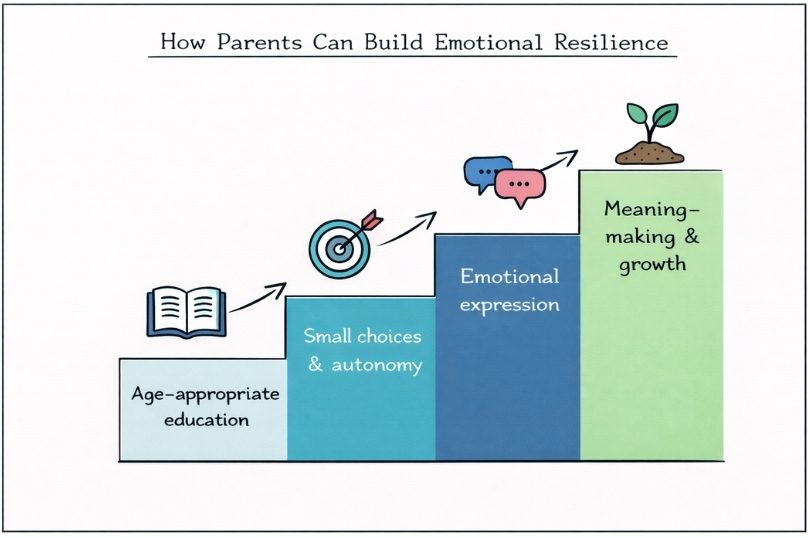
Autonomy development remains critical despite illness constraints. Providing children with age-appropriate choices regarding their care can make a big difference. Simple decisions, such as choosing where an injection is given, what flavour of medicine they prefer, or when to take their medication around meals, help them feel more in control. These small but meaningful choices can reduce feelings of helplessness that often come with living with a rare disease, and empower children to engage more confidently with their treatment.
Meaning-Making and Emotional Integration help children make sense of their illness, which is a powerful way to support emotional resilience. Activities that encourage meaning‑making, such as drawing, writing, storytelling, or open conversations, help children make sense of their medical experiences as part of their overall life story.
These expressions give parents and healthcare providers valuable insight into how the child understands their condition, highlighting any misconceptions that can then be gently corrected. By creating space for reflection and self‑expression, families help children transform difficult experiences into part of their personal growth journey.
Open communication channels form the cornerstone of psychological support. Studies show that children adjust better to difficult medical realities when they are given honest, age‑appropriate information. In contrast, parental secrecy often leads to misconceptions and increased anxiety.
Effective communication means listening as much as speaking, using active listening techniques that validate emotional experiences without rushing to solve the problem. Simple acknowledgment statements such as "that sounds really frustrating", "it makes sense that you'd feel scared," or “This is tough, isn’t it?” reassure children that their feelings are recognized and respected. This approach builds trust and creates a safe space for ongoing emotional expression.
Emotional vocabulary development enables children to articulate complex feelings related to their illness experience. When children can name and describe what they are experiencing, whether it’s fear, frustration, sadness, or anger, it becomes easier for them to express themselves and feel understood. Parents play a key role by modeling this process, sharing their own appropriate emotions, and demonstrating constructive ways to manage stress (“I’m feeling worried today, but I’m also hopeful”). This not only normalizes emotional expression but also shows children that it’s okay to talk about emotions and helps them learn healthy ways to cope.
Regular check-ins should occur beyond medical appointment discussions. Creating regular opportunities for open conversations about illness, whether during car rides, at bedtime, or in other quiet moments, helps normalize emotional expression. These routine check‑ins reassure children that support is always available and encourage them to share feelings consistently, rather than only in clinical settings.
Family system involvement for a child with a rare disease extends beyond parents or primary caregivers; it includes siblings, extended family, and close friends, all of whom play an important role in the child’s well-being. Each member of the support network needs some basic education about the child's condition and guidance on providing appropriate support without overprotection or unnecessary restrictions that could limit independence or emotional growth.
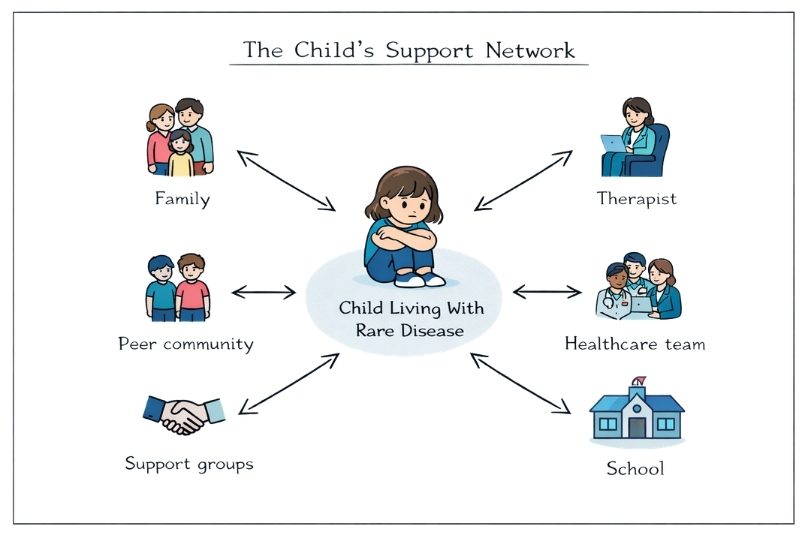
Building relationships with peers who are facing similar health challenges can significantly reduce feelings of isolation. Opportunities such as rare disease support networks, specialized camp programs, and online communities provide the child with spaces for genuine connection and understanding. These environments allow them to interact with others who truly grasp the realities of living with a chronic illness, helping normalize their experiences and fostering a sense of belonging. For additional mental health-focused resources and caregiver toolkits tailored to rare disease families, see Global Genes’ Mental Health Resources for the Rare Disease Community.
School collaboration is essential to ensure children receive consistent support across all areas of their lives. Developing a comprehensive school plan that addresses both academic accommodations and emotional support needs helps ensure your child feels supported at school as well as at home. When schools, families, and healthcare teams work together, your child is less likely to experience fragmented support that can increase anxiety and disrupt their learning or wellbeing.
A truly comprehensive healthcare team should include professionals with expertise in pediatric mental health and chronic illness. Child psychologists, social workers, and child life specialists bring specialized knowledge about how medical conditions affect the development and emotional well-being of children. Their evidence‑based strategies help children and families navigate the psychological challenges of illness while supporting healthy growth and resilience.
Therapeutic interventions may be necessary when your child shows persistent mood changes, behavioral regression, or significant difficulties in daily activities. Cognitive-behavioral therapy (CBT) is particularly effective for children living with chronic conditions, helping them develop healthy coping skills and gently change unhelpful thoughts that are related to their illness. By addressing both emotional and cognitive challenges, these interventions provide children with practical strategies to manage stress and strengthen resilience.
Family therapy addresses systemic impacts of rare disease on family dynamics and functioning. These interventions help families learn better ways to communicate, manage the stress that caregivers often feel, and maintain strong, healthy relationships even while facing the challenges of chronic illness. By working together in a structured setting, families can build resilience and maintain a supportive environment that benefits both the child and the entire household.
In some cases, a psychiatric consultation may be needed, particularly when children experience clinical depression, anxiety disorders, or other mental health conditions that require more intensive support. These consultations allow for careful evaluation and, when appropriate, the integration of medication management alongside psychological interventions. Families may also benefit from accessing specialist counselling for the rare disease community.
Crisis intervention planning should be established proactively, outlining clear steps before distress escalates. Families should proactively identify early warning signs of acute psychological distress, such as sudden withdrawal, intense anxiety, or thoughts of self-harm, and establish clear protocols for accessing emergency mental health services quickly.
While many emotional ups and downs are normal during a child’s illness, some signs suggest it may be time to seek professional mental health support.
Contact your child’s doctor or a mental health professional if your child shows any of the following for more than two weeks:

These behaviours often reflect underlying emotional distress rather than simple “bad behaviour.” Early support can make a big difference in helping your child feel better.
As adolescents transition into adult healthcare systems, continuity of mental health support is essential. This stage often brings new psychological challenges, as young people take on greater responsibility for managing complex medical care. Ongoing monitoring and tailored support plans help ensure that mental health needs are addressed, fostering resilience and easing the shift into adult care.
For more on this, read our practical guide on Transitioning From Paediatric To Adult Care, which explains why preparation should begin in early adolescence and how families can support a smoother transition while maintaining strong mental health support.
Talking openly about the future helps families balance realistic expectations with hopeful goal-setting. Children benefit from understanding that while their rare disease may shape certain aspects of their lives, it does not have to define their entire future. With the right support, they can envision opportunities and possibilities beyond their medical challenges, fostering resilience and a sense of agency in shaping their own life trajectory.
Resilience is not something children are born with; it is built through repeated success in navigating illness‑related challenges with the right support in place. Every time your child manages a difficult situation, whether it’s coping with a medical procedure, handling disappointment, or adapting to new limitations, they gain more confidence and emotional strength for the future.
Supporting a child’s mental health while living with a chronic rare disease requires sustained attention, professional collaboration, and evidence-based intervention strategies. Parents who prioritize psychological well-being alongside physical care create the best possible conditions for their child's overall development and long-term adjustment to life with a chronic condition.
The investment in comprehensive mental health support yields benefits that extend far beyond childhood; it helps build a strong foundation for lifelong resilience, equipping children to face ongoing health challenges with confidence and fostering enduring psychological well-being.