When your child has a rare disease, understanding all the available care options becomes essential for making informed healthcare decisions. Palliative and supportive care represent specialised medical services that focus solely on improving quality of life and managing symptoms, regardless of disease stage or prognosis. These approaches complement existing treatments and provide comprehensive support for both children and their families navigating complex medical journeys.
Palliative care is a medical speciality that primarily focuses on relief from symptoms and stress associated with serious illness. The World Health Organisation defines paediatric palliative care as the active total care of the child's body, mind, and spirit, involving support for the family. This approach usually begins at diagnosis and continues throughout the disease trajectory, with adaptations to meet changing needs over time.
For children with rare diseases, palliative care addresses multiple dimensions of care. Physical symptoms such as pain, fatigue, breathing difficulties, or feeding problems receive specialised attention through evidence-based interventions. The psychological and emotional aspects of living with chronic illness also receive focused support, recognising that rare diseases often create unique challenges for both children and their families.
Palliative care teams typically include paediatric specialists trained in symptom management, social workers, chaplains, child life specialists, and other healthcare professionals who understand the complex needs of children with serious illnesses. These interdisciplinary teams work collaboratively with existing medical providers to ensure coordinated, comprehensive care that addresses all aspects of the child's well-being.
Supportive care covers all interventions designed to prevent, manage, or treat the adverse effects of a disease and its treatments. In the context of rare diseases, supportive care often focuses on managing complications, optimising nutritional status, maintaining function, and preventing secondary conditions that might arise from the primary disease or its treatments.
The scope of supportive care extends beyond medical interventions to include educational support, rehabilitation services, and assistance with daily living activities. For families dealing with rare diseases, supportive care may involve helping children maintain participation in school, social activities, and age-appropriate developmental experiences despite medical challenges.
One of the most common misconceptions about palliative and supportive care involves timing and appropriateness. Both services can begin at any point after diagnosis and continue alongside curative or disease-modifying treatments. Research shows that early integration of palliative care improves quality of life, reduces unnecessary hospitalisations, and improves communication between families and medical teams.
For children with rare diseases, several indicators suggest potential benefits from palliative or supportive care services:
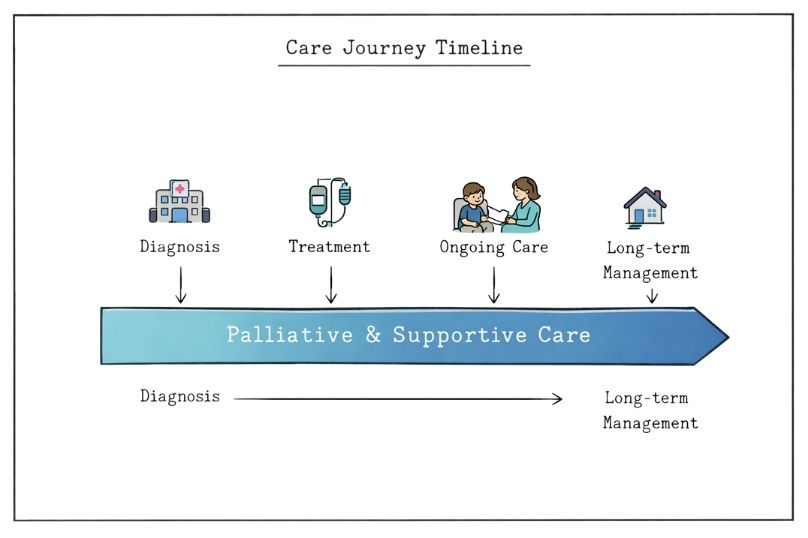
The process of accessing palliative and supportive care varies by healthcare systems and geographic location. In many cases, referrals come from existing medical providers who recognise the potential benefits of specialised services. However, families can also request these services directly, particularly when they identify unmet needs in symptom management or care coordination.
Paediatric palliative care programs exist in many major medical centres, with over 200 programmes operating across the United States, according to recent surveys. These programmes often provide both inpatient and outpatient services, allowing flexibility in how care is delivered. Some programmes offer home-based services, recognising that children with rare diseases may face challenges travelling to medical appointments.
Insurance coverage for palliative and supportive care services has improved significantly in recent years. Most major insurance plans now cover these services when provided by qualified teams, though specific coverage details vary by plan and provider. Families should work with insurance coordinators and social workers to understand coverage options and the potential out-of-pocket costs.
Palliative and supportive care teams approach care through comprehensive assessment and individualised planning. Initial evaluations typically include a detailed review of medical history, current symptoms, functional status, and family goals. Team members assess physical, psychological, social, and spiritual needs to develop coordinated care plans that address all relevant domains.
Communication represents a central focus of both palliative and supportive care. Teams prioritise clear and honest discussions about diagnosis, prognosis, treatment options, and the goals of care. For families dealing with rare diseases, where information may be limited or uncertain, these conversations help clarify and align care with family values and priorities.

Regular follow-up and care plan adjustments ensure that services remain consistent with changing needs and circumstances. As rare diseases often involve unpredictable disease trajectories, flexibility in care planning becomes crucial for maintaining appropriate support over time.
Many families express concern that pursuing palliative or supportive care indicates giving up hope or abandoning curative treatments. This misconception stems from the historical associations between palliative care and end-of-life services. Current practice standards emphasise that both palliative and supportive care complement ongoing medical treatments and do not require stopping disease-directed therapies.
Another common concern is whether these services are appropriate for children with uncertain prognoses, which frequently occurs with rare diseases. Both palliative and supportive care specifically address uncertainty by helping families handle complex medical decisions and maintain quality of life regardless of disease trajectory.
Rare diseases present unique challenges, making palliative and supportive care particularly valuable. Limited research and treatment options create uncertainty that can overwhelm families and medical teams. Specialised palliative care providers often have experience helping families manage medical uncertainty and make decisions with incomplete information.
The psychosocial impact of a rare disease diagnosis affects entire family systems. Siblings may experience neglect or anxiety, parents may face additional caregiver burden and financial stress, and extended family members may struggle to understand complex medical situations. Supportive care services tackle these broader impacts through family-centred interventions and resource coordination.
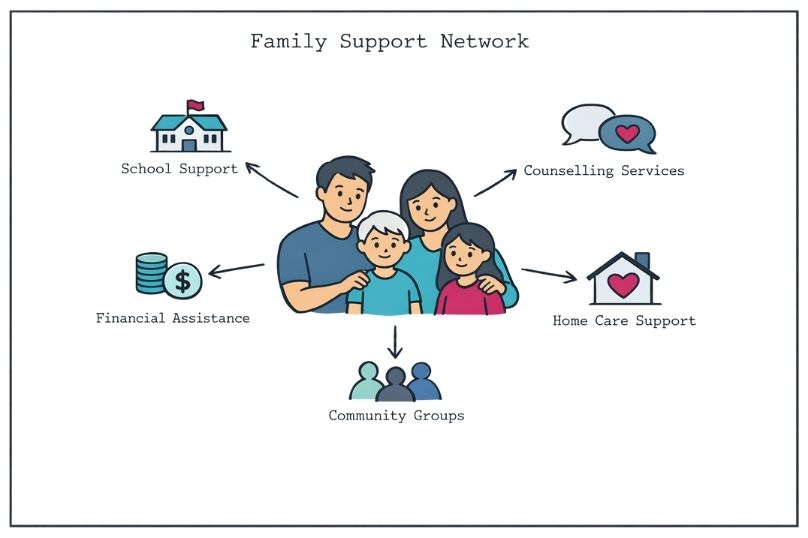
Successful palliative and supportive care requires integration with existing medical teams. Rather than replacing current providers, these services enhance care through specialised expertise in symptom management, communication facilitation, and care coordination. Many families find that palliative and supportive care teams help them navigate complex medical systems better and communicate more effectively with their existing providers.
Care coordination becomes particularly important when children receive care from multiple specialists, which is common with rare diseases. Palliative and supportive care teams often serve as central coordinators, helping ensure that all providers understand current goals, treatment plans, and family preferences.
As understanding of rare diseases continues to evolve, palliative and supportive care approaches also adapt to meet emerging needs. Advances in telemedicine have expanded access to specialised services, particularly for families in rural or underserved areas. Research into paediatric palliative care continues to refine best practices and exhibit improved outcomes for children and families.
The integration of palliative and supportive care principles into routine rare disease management displays an important trend in paediatric healthcare. Rather than waiting until crises occur, many medical centres now incorporate these approaches from the time of diagnosis, recognising their value in optimising outcomes and supporting family well-being throughout the disease journey.
Understanding available palliative and supportive care options empowers families to make informed decisions about their child's care. These services provide essential support and guidance for managing complex symptoms, mapping medical decisions, and maintaining quality of life while pursuing all appropriate treatment options for rare diseases.