Tay-Sachs disease is a rare inherited condition that affects the brain and nervous system. It belongs to a group of disorders known as lysosomal storage diseases, where the body is unable to properly break down certain substances inside cells.
Although the science behind Tay-Sachs can seem complex, the underlying idea is quite simple. The body normally has systems in place to break down and recycle materials. In Tay-Sachs disease, one of those systems does not work as it should. Over time, this leads to a gradual build-up of a fatty substance inside nerve cells, which eventually affects how those cells function.
This article explains what Tay-Sachs disease is, how it occurs, what symptoms can look like, and why genetic testing plays such an important role. The aim is to make the information clear, structured, and accessible without losing accuracy.
Tay-Sachs disease is caused by a change in a gene called the HEXA gene. This gene is responsible for producing part of an enzyme called beta-hexosaminidase A.
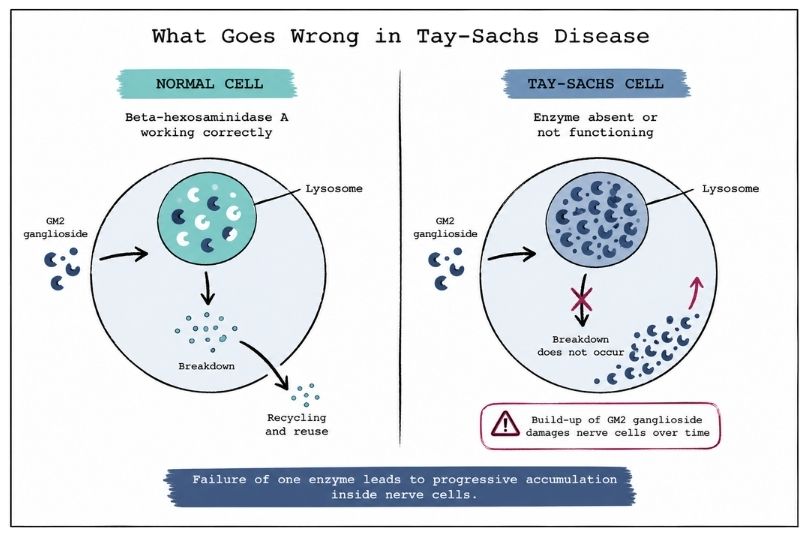
This enzyme has a very specific role. It helps break down a fatty substance called GM2 ganglioside, which is naturally found in nerve cells. Under normal conditions, the body carefully manages the levels of this substance.
When the HEXA gene does not function properly, the enzyme is either missing or not working effectively. As a result, GM2 ganglioside begins to accumulate inside nerve cells, particularly in the brain and spinal cord.
Over time, this build-up interferes with normal cell function and leads to progressive damage to the nervous system.
Tay-Sachs disease is inherited, which means it is passed through families via genes. It follows an inheritance pattern known as autosomal recessive.
This means:
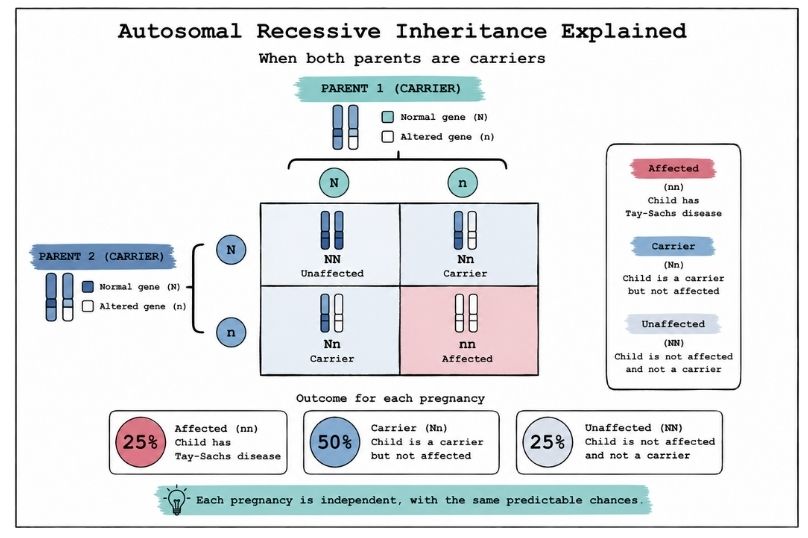
If a person has only one altered copy, they are known as a carrier. Carriers do not typically develop the disease because their second copy of the gene still works.
When both parents are carriers, there is a predictable pattern for each pregnancy:
| Outcome when both parents are carriers | Likelihood per pregnancy |
|---|---|
| Child develops Tay-Sachs disease | 25% |
| Child is a carrier (no disease) | 50% |
| Child is not affected and not a carrier | 25% |
These probabilities apply independently to each pregnancy.
Tay-Sachs disease can occur in any population. However, certain groups have historically had a higher chance of carrying the gene variation due to shared ancestry patterns.
These include:
Because of this, genetic screening programmes have often focused on these groups. However, modern genetic testing is increasingly offered more broadly, as ancestry alone does not capture all risk.
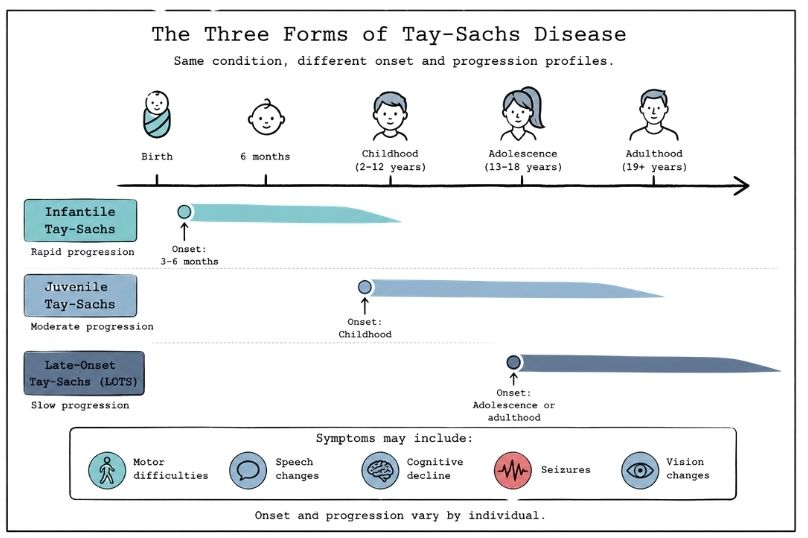
Tay-Sachs disease does not present in exactly the same way in every case. It is generally grouped into three forms based on when symptoms begin and how much enzyme activity remains.
| Form of Tay-Sachs | Typical Onset | General Pattern |
|---|---|---|
| Infantile | Around 3 to 6 months | Rapid progression |
| Juvenile | Childhood | Slower progression |
| Late-onset (adult) | Adolescence or adulthood | Much slower progression |
This is the most common and most severe form.
Babies with infantile Tay-Sachs usually appear typical at birth. Early development may also seem normal. Signs often begin to appear within the first few months of life.
Early features can include:
As the condition progresses, symptoms may include:
A characteristic clinical finding is a “cherry-red spot” seen during an eye examination. This is often one of the key indicators used in diagnosis.
Over time, the effects on the nervous system become more pronounced, and the condition leads to significant neurological impairment.
Juvenile Tay-Sachs is less common and typically appears later in childhood.
The progression is slower than the infantile form, but it still involves gradual neurological decline.
Symptoms may include:
Because symptoms appear later and can vary, diagnosis may take longer.
Late-onset Tay-Sachs (LOTS) is the rarest and mildest form.
It can begin in adolescence or adulthood and progresses much more slowly. Some individuals may live for many years with manageable symptoms.
Features may include:
Because the symptoms can overlap with other neurological conditions, this form is sometimes misdiagnosed initially.
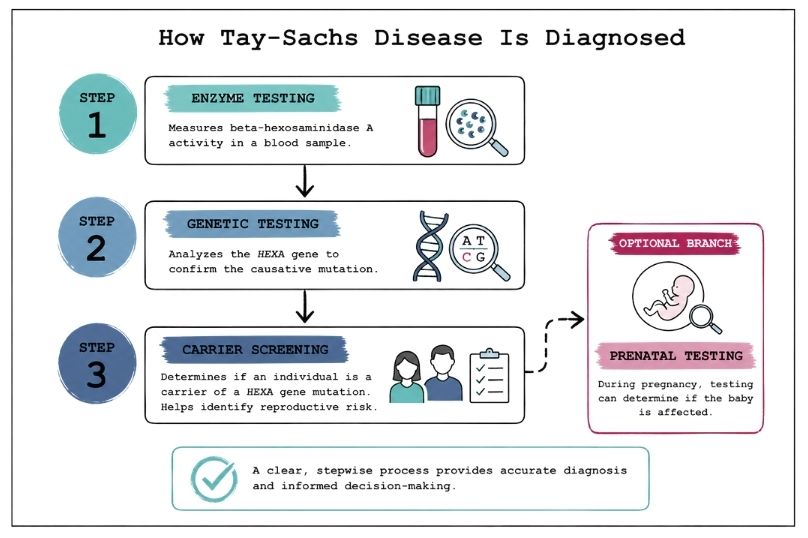
Diagnosis usually involves a combination of:
A blood test can measure the activity of beta-hexosaminidase A. Very low or absent activity strongly suggests Tay-Sachs disease.
Testing the HEXA gene can confirm the diagnosis and identify the specific genetic change.
This is often done before or during pregnancy to determine whether someone carries the gene.
Genetic testing plays a central role in Tay-Sachs disease because it provides clarity.
Carrier screening allows individuals and couples to:
Screening can be done before pregnancy or during early pregnancy. In some cases, prenatal testing may also be offered.
At present, there is no cure for Tay-Sachs disease.
Treatment focuses on supportive care, which aims to maintain comfort and quality of life. This may include:
Research is ongoing, including work in:
These areas are still under investigation and are not yet widely available as standard treatments.
For those who prefer visual explanations, the following videos provide clear, medically accurate overviews:
These explain both the biology of the condition and how it affects the body over time.
Because Tay-Sachs disease is rare, it is often misunderstood. A few clarifications can help:
Many neurological or developmental symptoms can have other causes. Tay-Sachs is only one possibility among many.
Medical information can sometimes feel overwhelming, particularly when symptoms seem to overlap with other conditions.
Tay-Sachs disease is very rare, and many of its symptoms are not specific to this condition alone. Developmental differences, neurological symptoms, or changes in behaviour can arise from a wide range of causes, most of which are far more common and often manageable.
Accurate diagnosis always relies on appropriate clinical assessment and, where relevant, targeted testing.
UK: https://rarediseasewatch.com/directory/the-cats-foundation/
USA: https://rarediseasewatch.com/directory/national-tay-sachs-allied-diseases-association-ntsad/
Tay-Sachs disease is a genetic neurological condition caused by changes in the HEXA gene. It leads to a build-up of GM2 ganglioside in nerve cells, resulting in progressive damage to the nervous system.
Key points:
Understanding Tay-Sachs disease helps place it in the correct context: a rare, clearly defined genetic condition with well-established diagnostic pathways.
Clarity is important, particularly when symptoms may overlap with other conditions. Structured information supports better understanding and more informed conversations in clinical settings.